What is a Tonometer?
The tonometer is a medical device used to measure intraocular pressure (IOP), to screen for and monitor serious conditions like glaucoma, where high IOP can damage the optic nerve. Tonometers work by gently flattening the cornea (applanation) or using a puff of air (non-contact) to gauge this internal pressure, helping doctors detect disease early and manage treatment. As such, tonometry is a fundamental part of routine eye exams, especially in optometry and ophthalmology clinics, hospitals, and screening programs.
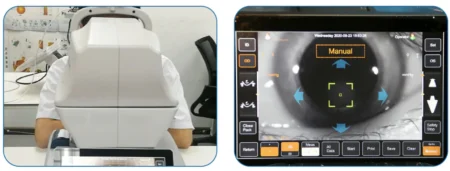
How Does a Tonometer Work?
Tonometers operate by assessing the resistance of the eye to an applied force. Various types exist, but the most common principles include:
- Applanation: Measures the force needed to flatten a small area of the cornea. The Goldmann Applanation Tonometer is the clinical gold standard.
- Indentation: Measures the depth of corneal indentation caused by a known weight.
- Non-contact (Air Puff): Uses a puff of air to flatten the cornea and measures the resulting deformation.
- Rebound: Uses a small probe that bounces off the cornea to estimate IOP.
Video demonstration:
Why Is Tonometer Accuracy Critical?
Accurate IOP measurements drive critical clinical decisions regarding diagnosis, treatment, and monitoring to prevent irreversible vision loss. Even slight IOP measurement errors can lead to:
- Missed glaucoma diagnosis (false low readings)
- Unnecessary treatment (false high readings)
Therefore, devices must be calibrated regularly and meet international safety standards. Reputable manufacturers—such as Shanghai LINK Instruments, certified under FDA, CE, ISO 13485, and ISO 9001—engineer tonometers with consistent precision for clinical reliability.
There are several different ways to measure eye pressure:
-
Goldmann Applanation Tonometer (The “Gold Standard”):
- How it works: This is the most accurate method. After numbing your eye with drops, the doctor gently touches a small, flat-tipped probe to the surface of your eye while you look through a slit lamp (microscope). It measures the force required to flatten a specific area of the cornea.
- Best for: Accurate diagnosis and management of glaucoma.
-
- How it works: This machine blows a gentle puff of air onto your eye to flatten the cornea slightly. It calculates pressure based on the air’s reflection and the eye’s resistance. It does not touch your eye, so no numbing drops are needed.
- Best for: Rapid screening, children, or patients who are squeamish about having their eyes touched.

-
Tono-Pen (Handheld):
- How it works: A portable, marker-sized device that the doctor touches gently to your numbed eye. It is very useful for patients who have trouble sitting at the slit lamp machine.
-
Rebound Tonometer (iCare):
- How it works: A handheld device that bounces a tiny, lightweight probe off the cornea very quickly. It happens so fast that you typically do not feel it, meaning no numbing drops are required.
- Best for: Children and patients with mobility issues.
Shanghai Link Instruments Co., Ltd. offers a range of high-quality tonometers and ophthalmic instruments that meet international standards such as ISO 9001, ISO 13485, CE, and FDA certifications. Their products support eye care professionals worldwide in delivering precise and reliable IOP measurements.
1. Is tonometry painful?
No, tonometry (eye pressure test) is generally not painful, though you might feel a brief puff of air or slight pressure, making you blink or jump, or a quick, light touch if anesthetic drops aren’t used.
2. How often should IOP be checked?
It depends on your risk for glaucoma, but generally, adults need it yearly after 40, while those with risk factors (family history, high pressure) need more frequent checks (every 3-6 months or sooner), with well-controlled glaucoma patients potentially going 6-12 months or longer between visits, as determined by your eye doctor for personalized management.
3. Can corneal thickness affect tonometer readings?
Yes, corneal thickness significantly affects tonometer readings; thicker corneas tend to overestimate intraocular pressure (IOP), while thinner corneas often underestimate it, especially with common methods like Goldmann applanation tonometry and air-puff devices, necessitating CCT (Central Corneal Thickness) measurement for accurate glaucoma assessment.
4. Are portable tonometers reliable?
Yes, portable tonometers (like
SW-1200A portable rebound or
SW-500 Handheld Tonometer) are generally reliable and very useful, especially for screening, children, or bedridden patients, offering portability and no anesthetic need.
5.What is a normal eye pressure for a tonometer?
A normal result means your eye pressure is within the normal range. The normal eye pressure range is 10 to 21 mm Hg.
6.What is the normal eye pressure for a 70 year old?
For a 70-year-old, normal eye pressure (IOP) generally falls within the standard adult range of 10 to 21 mmHg, though it may slightly decrease with age, often averaging around 14-15 mmHg in older adults, but the key is monitoring your personal baseline and optic nerve health, as a healthy nerve can tolerate higher pressure than a damaged one.
7.Is an eye pressure tonometer for home use accurate?
Yes,
home eye pressure tonometers (like the SW-500 HOME) are generally considered accurate and reliable for glaucoma monitoring, providing valuable data on daily fluctuations missed in clinics, but accuracy can vary by individual, with some studies showing potential overestimation at higher pressures or with thicker corneas, making physician guidance essential for interpreting results.







