Intraocular Pressure (IOP), with some of the most common metrics also being some of the least well-understood. Often compared to blood pressure in the eye, IOP serves as a basic indicator of ocular health. For clinicians, keeping IOP within an accepted physiological range is the main strategy to prevent permanent vision loss.
To understand what constitutes “normal” eye pressure, one must look beyond a simple numerical range. It requires an exploration of fluid dynamics, the precision of ophthalmic, optometry and optical lab equipment, and the anatomical variations that make every patient’s “normal” unique.
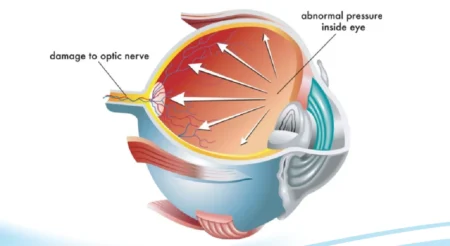
Why Is Eye Pressure Important for Ocular Health?
What Is Eye Pressure
Eye pressure, or intraocular pressure (IOP), is the fluid pressure inside the eye, maintained by a balance of fluid production and drainage. Normal eye pressure ranges from 10 to 21 mmHg.
Why Eye Pressure Matters
Eye pressure (intraocular pressure or IOP) is vital for ocular health because it maintains the eye’s shape, structural integrity, and proper function. A delicate balance of fluid (aqueous humor) production and drainage ensures this pressure stays within a normal range.
Key Aspects of Eye Pressure:
- Prevents Vision Loss: Consistently high eye pressure (ocular hypertension) can compress and damage the delicate optic nerve, which transmits visual information to the brain.
- Glaucoma Control: Elevated pressure is the primary risk factor for developing glaucoma, a leading cause of irreversible blindness.
- Structural Maintenance: The pressure is necessary for the eye to maintain its spherical shape, allowing for accurate focusing and vision.
- Detects Underlying Issues: Abnormally high or low pressure can signal underlying eye conditions such as inflammation, trauma, or previous surgery complications.
Key Considerations:
- Silent Threat: High eye pressure usually has no symptoms until permanent damage has occurred, making regular eye exams with tonometry crucial.
- Individual Thresholds: While 10–21 mmHg is considered normal, some individuals can develop glaucoma at “normal” pressures (normal-tension glaucoma), while others can tolerate higher pressures.
- Risk Factors: Age (over 40), family history, and high blood pressure can increase the risk of developing abnormal eye pressure.
- Regular eye exams, including pressure checks, are the best way to monitor this aspect of eye health.
What Is Normal Eye Pressure Range? (IOP)
- Below 10 mmHg: This is considered low (Hypotony). It can occur after eye surgery or trauma and may lead to blurred vision or structural changes in the globe.
- Above 21 mmHg: This is classified as ocular hypertension. While high pressure doesn’t automatically mean you have glaucoma, it is the primary risk factor that requires close monitoring.
Normal Eye Pressure for Adults?
Factors Affecting IOP:
- Circadian Rhythm: IOP typically peaks in the early morning hours and fluctuates throughout the day.
- Corneal Thickness: Thicker corneas can create artificially high readings, while thinner corneas can cause lower readings.
- Physical Position: Lying flat can slightly increase eye pressure compared to standing or sitting.
- Lifestyle Habits: Excessive caffeine consumption or extreme breath-holding during heavy weightlifting can cause temporary spikes.
Normal Eye Pressure for Seniors?
As we age, the risk profile for eye diseases shifts significantly. For seniors (those aged 60 and older), the definition of “normal” remains the same (12–21 mmHg), but the interpretation of those results becomes more critical.
Why Seniors Are at Higher Risk
- Increased Incidence of Glaucoma: The risk of developing glaucoma increases sixfold after age 60.
- Corneal Thinning: Many seniors experience changes in corneal thickness. A thinner cornea can lead to an “underestimation” of eye pressure during a test, meaning the actual pressure is higher than what the machine displays.
How Is Eye Pressure Measured and Monitored?
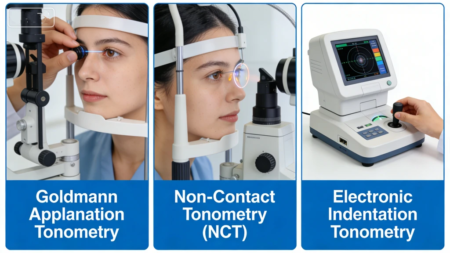
- Goldmann Applanation Tonometry: Often considered the “gold standard,” this involves a small probe gently pressing against the cornea (following numbing drops). It is usually performed using a Slit Lamp.
- Non-Contact Tonometry (NCT): Commonly known as the “air puff” test. This is a non-invasive way to screen large numbers of patients quickly and is ideal for initial assessments in busy optical centers.
- Electronic Indentation Tonometry: Portable devices that are useful for patients who may have difficulty sitting at a traditional station.
How to Keep Eye Pressure Within the Healthy Range?
Key Lifestyle Changes for Healthy Eye Pressure:
- Regular Exercise: Engage in moderate aerobic activity like brisk walking, cycling, or swimming 3-4 times a week.
- Sleep Position: Use a wedge pillow to keep your head slightly elevated while sleeping to reduce nighttime pressure.
- Dietary Adjustments: Eat foods rich in antioxidants and vitamins A, C, and E, such as leafy greens (spinach, kale), berries, and fish high in omega-3 fatty acids (salmon, tuna).
- Limit Caffeine: Excessive caffeine (more than 3-5 cups daily) can temporarily increase IOP. Limit coffee and tea consumption.
- Avoid Smoking: Smoking cigarettes or using tobacco increases IOP and harms the optic nerve.
- Manage Stress: Practice relaxation techniques such as meditation or yoga to reduce stress, which can trigger spikes in IOP.
Activities to Avoid (if you have high IOP)
1. Physical Activities
- Heavy weightlifting (avoid breath-holding / Valsalva)
- Inverted positions (head below heart, e.g., headstands)
- High-impact/contact sports (eye injury risk)
- Tight swimming goggles
2. Lifestyle & Daily Habits
- Excess caffeine intake
- Drinking large amounts of water quickly
- Prolonged bending / head-down posture
- Tight collars or neckties
- Sleeping face-down (eye pressure)
- Unsupervised steroid use
Tip: Prefer moderate aerobic exercise (walking, cycling) to help lower IOP.
Which Warning Signs Should You Watch For?
- Severe eye pain or headache.
- Nausea or vomiting.
- Seeing “halos” or rainbow-colored rings around lights.
- Blurred vision or sudden loss of sight.





